Mitral regurgitation (MR), a “leaky” mitral valve, is the most common type of heart valve disease. Some people with MR often have no symptoms and can remain stable for many years and often for their whole lives. However, in other people, MR eventually produces decompensation of the heart, and heart failure results. In such cases, heart failure may not be reversible.
The trick to preventing heart failure with MR is to recognize the time when the heart is beginning to decompensate, but before symptoms of heart failure occur.
So if you have MR it is very important that you have regular checkups with your doctor to determine the extent of your MR, and to see whether your condition is stable or whether it is getting worse. This process is called 'staging' MR.
Determining the stage of MR can help you and your doctor decide whether you may need surgical therapy, and, very importantly, to determine the optimal time for surgical therapy should you require it.
The Stages of Chronic Mitral Regurgitation
Cardiologists divide chronic MR into three 'stages.' Determining the stage of your MR helps your cardiologist to decide whether and when mitral valve surgery may be needed.
The Compensated Stage. In the compensated stage of MR, the heart and the cardiovascular system has “adjusted” to the extra volume load placed on the left ventricle by the damaged valve. The heart compensates by enlarging somewhat, but the dilated heart muscle is otherwise functioning normally. People with compensated MR generally report no symptoms, though their exercise capacity generally turns out to be reduced if a stress test is performed. Many patients with mild, chronic MR remain in the compensated stage throughout their lives.
The Transitional Stage. For reasons that are not clear, some people with MR will gradually “transition” from a compensated to a decompensated condition. Ideally, valve repair surgery should be performed during this transitional stage, when the risk of surgery is relatively low and the results relatively good.
In the transitional stage the heart begins to enlarge, cardiac pressures rise, and the ejection fraction falls. While patients in this stage are more likely to report symptoms of dyspnea and poor exercise tolerance, many don’t notice worsening symptoms until their MR has progressed to the third stage. This is a problem, since delaying surgery until the decompensated stage is likely to yield a poor outcome.
Many experts believe once atrial fibrillation occurs in the presence of MR, especially if it is associated with dilation of the left atrium, that fact alone ought to indicate that the transitional stage has arrived, and therefore, that valve repair surgery ought to be at least considered.
The Decompensated Stage. Patients in the decompensated stage almost invariably have very considerable cardiac enlargement, as well as significant symptoms of heart failure. Once the decompensated stage has occurred, cardiomyopathy (damage to the heart muscle ) is present and will remain present even if the mitral valve is repaired. So valve repair surgery becomes quite risky and is not likely to produce an acceptable result.
The Importance of Staging MR
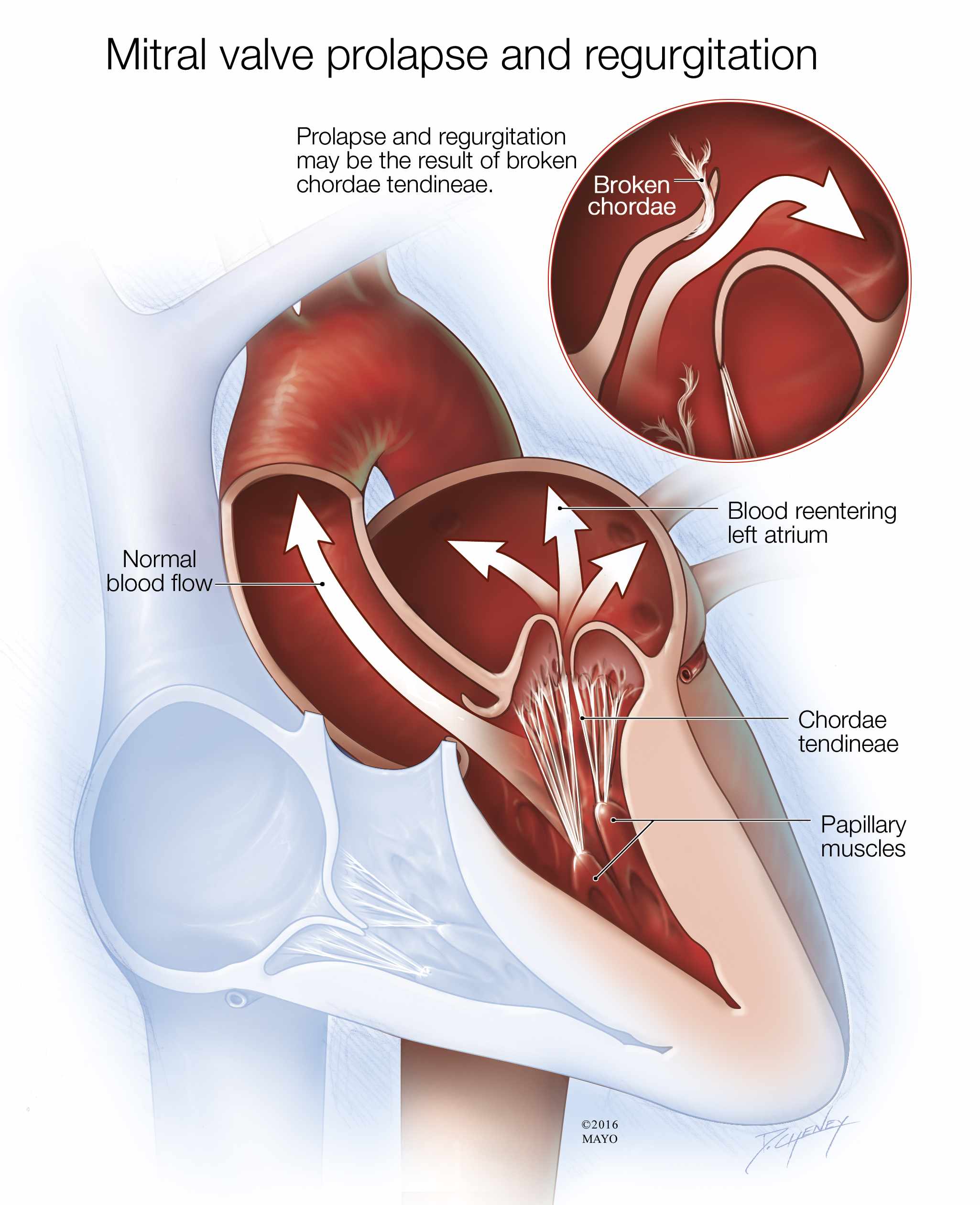
In mitral valve prolapse, the leaflets of the mitral valve bulge (prolapse) into the left atrium like a parachute during the heart's contraction. Sometimes mitral valve prolapse causes blood to leak back into the atrium from the ventricle, which is called mitral valve regurgitation.
It is critically important to 'catch' the transitional stage of MR before it progresses to the decompensated stage. For this reason, if you have MR you need to have close medical monitoring. Among other things, it is important for your doctor to carefully evaluate whether any new symptoms you may be experiencing are due to MR. In addition, periodic echocardiograms are needed to help your doctor to assess the state of your mitral valve and cardiac chambers.
If you have MR, you should make sure your doctor is doing this appropriate monitoring — and you yourself need to pay close attention to any signs of shortness of breath, or a reduced ability to exert yourself.
- Bonow, RO, Carabello, BA, Chatterjee, K, et al. 2008 Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Circulation 2008; 118:e523.
- Vahanian, A, Baumgartner, H, Bax, J, et al. Guidelines on the management of valvular heart disease: The Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology. Eur Heart J 2007; 28:230.
The mitral valve is located in the left side of your heart between two chambers: the left atrium and the left ventricle. The valve works to keep blood flowing properly in one direction from the left atrium to the left ventricle. It also prevents blood from flowing backward.
Mitral valve disease occurs when the mitral valve doesn’t work properly, allowing blood to flow backward into the left atrium. As a result, your heart does not pump enough blood out of the left ventricular chamber to supply your body with oxygen-filled blood. This can cause symptoms such as fatigue and shortness of breath. However, many people with mitral valve disease experience no symptoms.
If left untreated, mitral valve disease can lead to serious, life-threatening complications such as heart failure or irregular heartbeats, called arrhythmias.
There are three types of mitral valve disease: stenosis, prolapse, and regurgitation.
Mitral valve stenosis
Stenosis occurs when the valve opening becomes narrow. This means that not enough blood can pass into your left ventricle.
Mitral valve prolapse
Prolapse occurs when the flaps on the valve bulge instead of closing tightly. This might prevent the valve from closing completely, and regurgitation — the backward flow of blood — may occur.
Mitral valve regurgitation
Regurgitation occurs when blood leaks from the valve and flows backward into your left atrium when the left ventricle compresses.
Each form of mitral valve disease has its own set of causes.
Mitral valve stenosis
Mitral valve stenosis is typically caused by scarring from rheumatic fever. Usually a childhood disease, rheumatic fever results from the body’s immune response to a streptococcal bacterial infection. Rheumatic fever is a serious complication of strep throat or scarlet fever.
The organs most affected by acute rheumatic fever are the joints and the heart. The joints can become inflamed, which can lead to temporary and sometimes chronic disability. Various parts of the heart can become inflamed and lead to these potentially serious heart conditions, including:
- endocarditis: inflammation of the lining of the heart
- myocarditis: inflammation of the heart muscle
- pericarditis: inflammation of the membrane surrounding the heart
If the mitral valve becomes inflamed or otherwise injured by these conditions, it can lead to the chronic heart condition called rheumatic heart disease. The clinical signs and symptoms of this condition might not occur until 5 to 10 years after the episode of rheumatic fever.
Mitral stenosis is uncommon in the United States and other developed countries where rheumatic fever is rare. This is because people in developed countries generally have access to antibiotics that treat bacterial infections such as strep throat, according to the Merck Manual Home Health Handbook. Most cases of mitral stenosis in the United States are in older adults who had rheumatic fever before the widespread use of antibiotics or in people who have moved from countries where rheumatic fever is common.
There are other causes of mitral valve stenosis, but these are rare. They include:
- calcium buildup
- tumors
Mitral valve prolapse
Mitral valve prolapse often has no specific or known cause. It tends to run in families or occur in those who have other conditions, such as scoliosis and connective tissue problems. According to the American Heart Association, about 2 percent of the U.S. population has a mitral valve prolapse. Even fewer people experience serious problems associated with the condition.
Mitral valve regurgitation
A variety of heart problems can cause mitral valve regurgitation. You may develop mitral valve regurgitation if you’ve had:
- endocarditis, or inflammation of the heart’s lining and valves
- rheumatic fever
Damage to your heart’s tissue cords or wear and tear to your mitral valve can also lead to regurgitation. Mitral valve prolapse can sometimes cause regurgitation.
Mitral valve disease symptoms vary depending on the exact problem with your valve. It may cause no symptoms at all. When symptoms do occur, they can include:
- cough
- shortness of breath, especially when you’re lying down on your back or exercising
- fatigue
- lightheadedness
You may also feel pain or tightness in your chest. In some cases, you might feel your heart beating irregularly or quickly.
Symptoms of any type of mitral valve disease usually develop gradually. They might appear or get worse when your body is dealing with extra stress, such as infection or pregnancy.
If your doctor suspects that you may have a mitral valve disease, they will listen to your heart with a stethoscope. Unusual sounds or rhythm patterns can help them diagnose what’s going on.
Your doctor may order additional tests to help confirm a mitral valve disease diagnosis.
Imaging tests
- Echocardiogram: This test uses ultrasound waves to produce images of the heart’s structure and function.
- X-ray: This common test produces images on computer or film by sending X-ray particles through the body.
- Transesophageal echocardiogram: This test produces a more detailed image of your heart than a traditional echocardiogram. During the procedure, your doctor threads a device emitting ultrasound waves into your esophagus, which is located right behind the heart.
- Cardiac catheterization: This procedure allows your doctor to do a variety of tests, including getting an image of the heart’s blood vessels. During the procedure, your doctor inserts a long, thin tube into your arm, upper thigh, or neck and threads it up to your heart.
- Electrocardiogram (ECG or EKG): This test records your heart’s electrical activity.
- Holter monitoring: This is a portable monitoring device that records your heart’s electrical activity over a period of time, usually 24 to 48 hours.
Tests to monitor heart activity
Stress tests
Your doctor may want to monitor you while you exercise to determine how your heart responds to physical stress.
Treatment for mitral valve disease may not be necessary, depending on the severity of your condition and symptoms. If your case is severe enough, there are three possible treatments or combination of treatments that may correct your condition.
Drugs and medication
If treatment is necessary, your doctor may begin by treating you with medications. There are no medications that can actually fix the structural issues with your mitral valve. Some medications can ease your symptoms or prevent them from getting worse. These medications may include:
- antiarrhythmics, to treat abnormal heart rhythms
- anticoagulants, to thin your blood
- beta blockers, to slow your heart rate
- diuretics, to reduce accumulation of fluid in your lungs
Valvuloplasty
In some cases, your doctor may need to perform medical procedures. For example, in cases of mitral valve stenosis, your doctor may be able to use a balloon to open up the valve in a procedure called balloon valvuloplasty.
Surgery
In severe cases, surgery might be necessary. Your doctor might be able to surgically repair your existing mitral valve to make it function properly. If that isn’t possible, you may need to have your mitral valve replaced with a new one. The replacement might be either biological or mechanical. The biological replacement might be obtained from a cow, pig, or human cadaver.
When the mitral valve does not function as it should, your blood does not flow properly out of the heart. You may experience symptoms such as fatigue or shortness of breath, or you may not experience symptoms at all. Your doctor will use a variety of tests to diagnose your condition. Treatment may involve a variety of medications, medical procedures, or surgery.
